The Medicine Cabinet Purge That Costs Billions
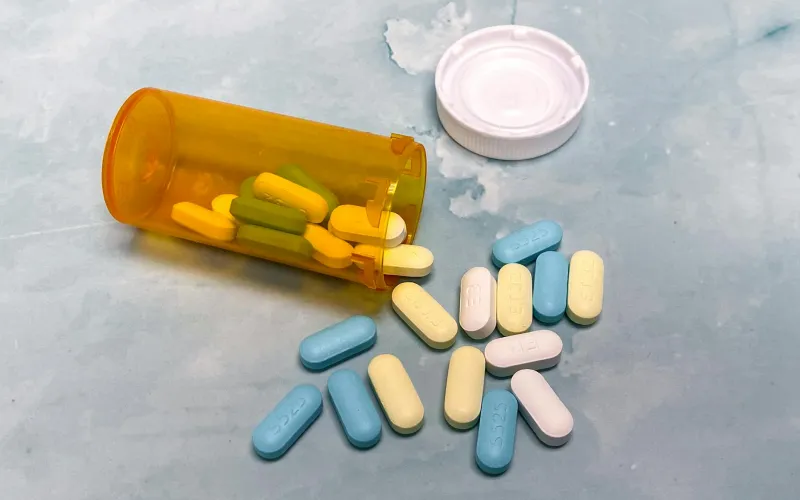
Every year, American households perform the same ritual: checking medicine cabinets for expired bottles and tossing anything past its printed date. It feels responsible, maybe even necessary for safety. But this nationwide purge wastes an estimated $5 billion in perfectly good medication annually, based on dates that measure something entirely different than what most people think.
The expiration date stamped on your prescription bottle doesn't mark when the drug becomes dangerous. It marks when the manufacturer can no longer guarantee the medication will be 100% as potent as labeled. That's a crucial distinction that most patients — and surprisingly, many doctors — don't fully understand.
What the Military Discovered About Old Pills
The most comprehensive research on medication longevity didn't come from pharmaceutical companies or medical schools. It came from the U.S. military, which faced a practical problem: stockpiled medications worth hundreds of millions of dollars were approaching their expiration dates.
 Photo: U.S. military, via images-wixmp-ed30a86b8c4ca887773594c2.wixmp.com
Photo: U.S. military, via images-wixmp-ed30a86b8c4ca887773594c2.wixmp.com
Starting in the 1980s, the Department of Defense partnered with the FDA to create the Shelf Life Extension Program. Instead of automatically discarding expired drugs, they tested them. The results were striking: 90% of medications retained their full potency for at least one year beyond expiration, and many remained effective for much longer.
 Photo: Department of Defense, via techcrunch.com
Photo: Department of Defense, via techcrunch.com
Some antibiotics tested by the program were still 100% potent after 15 years. Heart medications, pain relievers, and allergy drugs consistently showed minimal potency loss even years past their printed dates. The military has saved over $3 billion by using these findings to extend the shelf life of their medical supplies.
The Business of Expiration Dating
So why don't pharmaceutical companies test their drugs for longer periods? The answer lies in FDA regulations established in the 1970s. When a company wants to market a new medication, they must prove how long it remains stable and potent. But there's no requirement to test beyond what they plan to claim.
Testing costs money and time. A company might test their new blood pressure medication for two years and find it's still perfectly good — but why spend additional resources testing for five or ten years when two years is sufficient to get FDA approval and start selling?
Shorter expiration dates also create a predictable replacement cycle. Patients refill prescriptions more frequently, pharmacies restock more often, and pharmaceutical companies maintain steady revenue streams. It's a system that works well for everyone except the people actually paying for the medication.
The Real Risks Worth Knowing
This doesn't mean every expired medication is safe to use indefinitely. Some drugs do lose potency more quickly, and a few can become genuinely dangerous over time.
Tetracycline, an antibiotic, can break down into compounds that damage kidneys. Insulin loses effectiveness relatively quickly, especially if not stored properly. Liquid medications and anything requiring refrigeration typically have shorter true shelf lives than their solid counterparts.
The bigger concern isn't usually safety — it's effectiveness. Taking a pain reliever that's lost 20% of its potency might mean your headache doesn't fully resolve. Using expired emergency medications like epinephrine auto-injectors could be life-threatening if they don't deliver their full dose.
Why Doctors Often Don't Know
Most physicians receive little training about medication stability and storage. They learn about prescribing, dosing, and side effects, but the shelf life science typically isn't covered in medical school. Many doctors genuinely believe expired medications become dangerous, because that's the message they've absorbed from pharmaceutical marketing and medical culture.
Pharmacists generally know more about drug stability, but they're also legally required to recommend following manufacturer guidelines. Few are willing to suggest patients ignore expiration dates, even when the science suggests it might be safe.
The Storage Factor That Actually Matters
While expiration dates get all the attention, how you store medication affects its longevity far more than time alone. Heat, humidity, and light break down drugs much faster than simple aging.
That medicine cabinet in your bathroom — warm and steamy from showers — is actually one of the worst places to store pills. A cool, dry, dark location maintains potency much better. Many medications stored properly will outlast their expiration dates, while the same drugs stored in poor conditions might lose effectiveness before they expire.
What This Means for Your Medicine Cabinet
The military research suggests that most solid medications — tablets, capsules, pills — remain safe and effective well beyond their printed dates when stored properly. But individual circumstances matter. Someone managing a chronic condition with precise dosing requirements faces different risks than someone taking occasional over-the-counter pain relievers.
The current system errs heavily on the side of caution, which isn't necessarily wrong. But understanding what expiration dates actually measure can help you make more informed decisions about medication waste, emergency preparedness, and when those dates truly matter for your health.
The next time you're cleaning out your medicine cabinet, remember: that date on the bottle is measuring guaranteed potency, not safety. The military has been proving that distinction for decades.